A drug-resistant and potentially deadly fungus has been spreading rapidly through U.S. health care facilities, a new government study finds.
The fungus, a type of yeast called Candida auris, or C. auris, can cause severe illness in people with weakened immune systems. The number of people diagnosed with infections — as well as the number of those who were found through screening to be carrying C. auris — has been rising at an alarming rate since it was first reported in the U.S., researchers from the Centers for Disease Control and Prevention reported Monday.
The increases, “especially in the most recent years, are really concerning to us,” the study’s lead author, Dr. Meghan Lyman, chief medical officer in the CDC’s Mycotic Diseases Branch, said in an interview. “We’ve seen increases not just in areas of ongoing transmission, but also in new areas.”
The CDC’s new warning, published in the Annals of Internal Medicine, comes as Mississippi is fighting a growing outbreak of the fungus. Since November, at least 12 people have been infected with C. auris with four “potentially associated deaths,” according to the state’s health department, Tammy Yates, spokesperson for Mississippi State Department of Health said in an email.
There has been ongoing transmission at two long-term care facilities, although cases have been identified at several other facilities in the state.
“Unfortunately, multi-drug resistant organisms such as C. auris have become more prevalent among our highest risk individuals, such as residents in long-term care facilities,” said Yates.
The fungus can be found on the skin and throughout the body, according to the CDC. It’s not a threat to healthy people, but about one-third of people who become sick with C. auris die.
In the CDC report, researchers analyzed state and local health department data on people sickened by the fungus from 2016 through Dec. 31, 2021, as well as those who were “colonized,” meaning they were not ill but were carrying it on their bodies with the potential of transmitting it to others who might be more vulnerable to it.
The number of infections increased by 59%, to 756, from 2019 to 2020 and then by an additional 95%, to 1,471, in 2021.
The researchers also found that the incidence of people not infected with the fungus but colonized by it increased by 21% in 2020, compared to 2019, and by 209% in 2021, with an increase to 4,041 in 2021 compared to 1,310 in 2020.
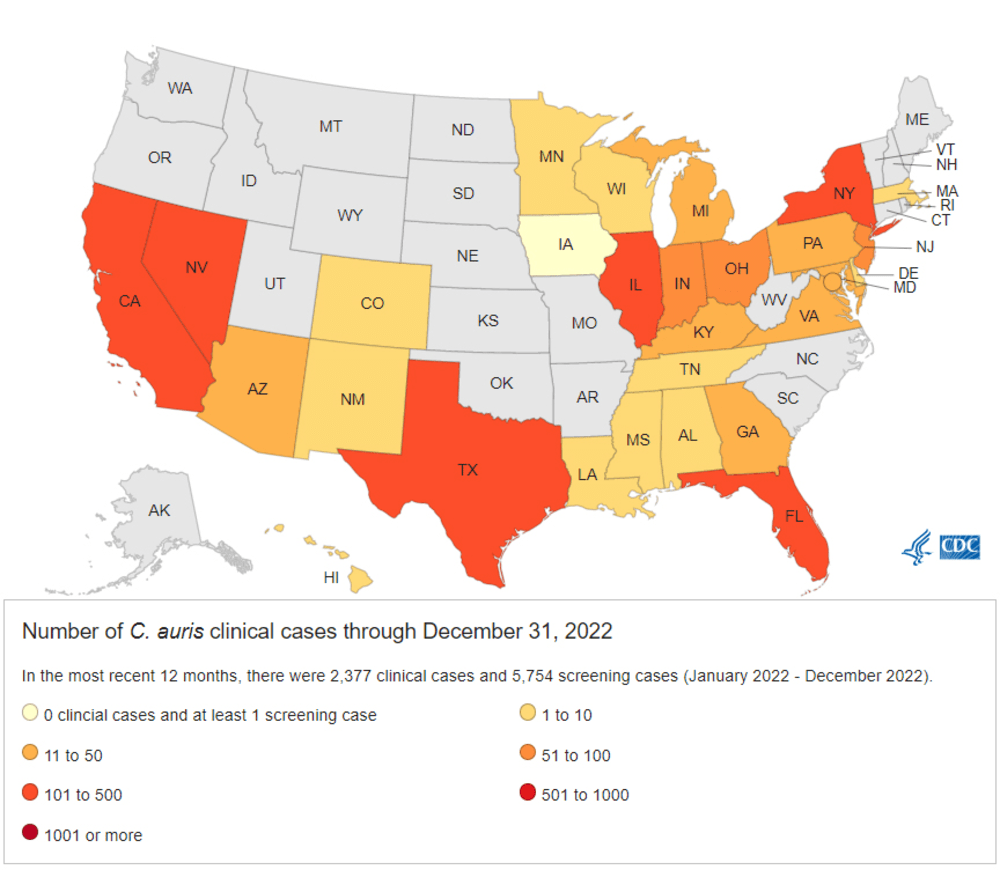
C. auris has now been detected in more than half of U.S. states, the new study found.
Most concerning was the increasing numbers of fungus samples resistant to the common treatments for it. Lyman hopes the paper will put C. auris on health care providers’ radar and spur facilities to practice “good infection control.”
The new findings are “worrisome,” said Dr. Waleed Javaid, an epidemiologist and an infectious disease expert and director of infection prevention and control at Mount Sinai Downtown in New York.
“But we don’t want people who watched ‘The Last of Us’ to think we’re all going to die,” Javaid said. “This is an infection that occurs in extremely ill individuals who are usually sick with a lot of other issues.”
Even if C. auris moves beyond health care facilities and into communities, it’s unlikely to become a problem for healthy people who do not have invasive medical devices, such as catheters, inserted into their blood vessels, Javaid said.
The main problem is preventing the fungus from spreading to patients in hospital intensive care units, Javaid said. Unfortunately C. auris can colonize not only people who come in contact with the fungus, but also patient rooms.
“By its nature it has an extreme ability to survive on surfaces,” he said. “It can colonize walls, cables, bedding, chairs. We clean everything with bleach and UV light.”
While the fungus was first identified in 2009 in Asia, scientists have determined that C. auris first appeared around the world about a decade earlier, after they re-examined older data and discovered instances where C. auris had been mistakenly identified as a different fungus, Dr. Graham Snyder, medical director of infection prevention at University of Pittsburgh Medical Center, said in an interview.
“It’s the pattern we’ve observed with these types of pathogens,” he said. “Often they start out extremely rare, then they emerge in more and more places and become widespread.”
It’s important to stop the pathogen so it doesn’t spread beyond hospitals and long-term facilities like the drug-resistant bacteria MRSA did, Snyder said.
“It’s not unusual to see MRSA in the community now,” Snyder said. “Will that happen with C. auris? I don’t know. That’s partly why the CDC is raising the alarm.”