
Twenty-four hours after hearing her six-year-old son likely had leukaemia, a Perth mother was told he was being removed from her care.
It’s a scenario the single mum-of-two said was “a living nightmare” that began after a GP visit in January when she saw blood in her son’s stool and asked for tests to rule out anything serious. She was told to go to hospital.
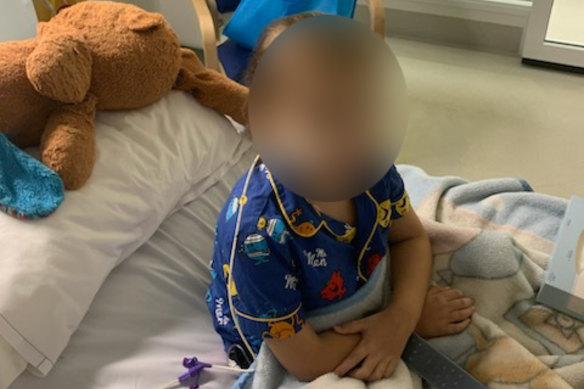
Jenny* said a meeting with an oncologist at Perth Children’s Hospital two days later turned argumentative.
“We asked for test results but weren’t given anything,” Jenny said.
“We’d seen no paperwork. They just took us into this little room and explained that he has probably got leukaemia and this is what the treatment is.

“I said I wanted a second opinion, I wanted to explore all my options and maybe take him home for a few days before he starts any treatment.”
Department of Communities documents stated the mother allowed fluids and medications to be given to her son, but asked to take him home for the night and bring him back the following day for a bone marrow sample to be taken.
The hospital would not allow this, warning there was a high risk of sepsis if he got an infection outside hospital.
Jenny disputed claims in the documents that she told hospital staff she would refuse chemotherapy and instead treat him homeopathically.
“We’re not hippies, we weren’t going to run away into the bush and give him blueberries and not accept that he’s got leukaemia,” she said.
“I just wanted to know everything that I could and we just wanted to give our brains a chance to comprehend what we were hearing.
“I’m not anti-chemo, I just wanted it to be my choice for my child and for my family.”
Instead, Jenny alleged the oncologist told her she would “red flag” her to the Department of Child Protection if James* was removed from the hospital, telling her he could get an infection and “be dead within 60 minutes”.
WAtoday is not using the family’s real names, as children in care cannot legally be identified.
“I just broke down hysterically,” Jenny said.
“I couldn’t believe what I was hearing.
“I told them to call DCP, that I wanted to talk to them myself. I wasn’t worried because I knew I had done nothing wrong.”
Later that day, Jenny said she, her younger son and her mother were locked out of the ward where James was staying and forced to leave the hospital without him.
She was served with a section 37 order, which gave DCP employees the power to take a child into provisional care “if the officer suspects on reasonable grounds that there is an immediate and substantial risk to the child’s wellbeing”.
After two months in hospital receiving chemotherapy, James was placed in foster care more than an hour’s drive from his Hamilton Hill home and enrolled into a new school.
Jenny is only allowed to see him for short supervised visits and has been banned from attending any of his ongoing treatment appointments at PCH.
He has not seen his three-year-old brother or grandmother since his diagnosis.
Legal fight launched
Court documents revealed the DCP was attempting to keep James under the care of the state for two years while his treatment continues, citing neglect as the reason.
“The parents [are] unable to provide or arrange effective medical, therapeutic, or other remedial treatment for the child or risk of that,” the documents stated.
Perth Children’s Hospital staff called the department on the same day Jenny was told about James’ leukaemia and treatment plan.
In explaining why James was removed from his mother’s care, the documents said: “[PCH was] concerned that [the child’s mother and grandmother] were threatening to discharge [the child] against medical advice. [Jenny] presented very hostile and aggressive. [The grandmother] was described as ‘very obstructive and pathological’ as she raised her voice and talked over staff at Perth Children’s Hospital.”

Both women denied the allegations and claimed they only ever wanted a second opinion and to explore alternative treatments that could be used in conjunction with chemotherapy.
“I hadn’t even been allowed to adjust and accept that my child was sick,” Jenny said.
“I was just angry at that point. There was going to be no trust. I asked for a different doctor. I asked for his drip to be taken out so I could take him and things got a little heated, and I was yelling and upset but not once did I ever refuse any treatment.
“I just wanted to take him somewhere else but there.
“It was already horrendous what was being done, I didn’t want any more of it.
“We tried to communicate, tried to come to an agreement, but we weren’t getting anywhere.”
They claimed an oncologist at the hospital would not allow them to get a second opinion from outside the hospital.
The women claimed they asked staff if James could be relocated to Fiona Stanley Hospital for a few days to be closer to their home, making it easier for the whole family to be with him while they looked at options.
They also claimed his risk of a life-threatening infection leading to death would have been mitigated by living just seven minutes’ drive from the hospital, and that at the time James was “doing cartwheels” and looking as healthy as ever.
Allegedly, at no time were they offered any counselling or support services.
The case is now before Perth Children’s Court, where a judge will decide whether James continues his treatment in the care of his family or with a foster family.
Jenny said DCP had stated she must “work with the hospital” if she was to have her parental rights reinstated, but claimed she has been repeatedly asking for test results, meetings with the treatment team, and information about her son’s situation since January.
Child and Adolescent Health Service chief executive Valeria Jovanovic said quality care and patient safety was the “highest priority at Perth Children’s Hospital”.
“At all times the child, and their families and carers, are at the centre of all clinical decisions,” she said.
“Our clinical care is based on national and international guidelines and treatment protocols. Should there be an occasion where a family would like to seek a second opinion from another team in an appropriate relevant clinical speciality, we are happy to facilitate this.”
A Department of Communities spokesperson said the safety and wellbeing of children is “always the Department of Communities’ top priority”.
“In keeping with its legal obligations, Communities does not comment on individual cases,” he said.
*Names have been changed for legal reasons.



