ABSTRACT
BACKGROUND There were increased SARS-CoV2 hospitalizations and deaths noted during Omicron (B.1.1.529) variant surge in UK despite decreased cases, and the reasons are unclear.
METHODS In this observational study, we analyzed reported SARS-CoV2 cases, hospitalizations and deaths during the COVID-19 pandemic in the UK. We also analyzed variables that can affect the outcomes. The vaccine effectiveness among those ≥18 years of age (August 16, 2021 to March 27, 2022) was analyzed.
RESULTS Of the total cases (n= 22,072,550), hospitalizations (n=848,911) and deaths (n=175,070) due to COVID-19 in UK; 51.3% of cases (n=11,315,793), 28.8% of hospitalizations (n=244,708) and 16.4% of deaths (n=28,659) occurred during Omicron variant surge. When comparing the period of February 28-May 1, 2022 with the prior 12-weeks, we observed a significant increase in the case fatality rate (0.19% vs 0.41%; RR 2.11 [2.06-2.16], p<0.001) and odds of hospitalization (1.58% vs 3.72%; RR 2.36[2.34-2.38]; p<0.001). During the same period a significant increase in cases (23.7% vs 40.3%; RR1.70 [1.70-1.71]; p<0.001) among ≥50 years of age and hospitalizations (39.3% vs 50.3%;RR1.28 [1.27-1.30]; p<0.001) and deaths (67.89% vs 80.07%;RR1.18 [1.16-1.20]; p<0.001) among ≥75 years of age was observed. The vaccine effectiveness (VE) for the third dose was in negative since December 20, 2021, with a significantly increased proportion of SARS-CoV2 cases hospitalizations and deaths among the vaccinated; and a decreased proportion of cases, hospitalizations, and deaths among the unvaccinated. The pre-existing conditions were present in 95.6% of all COVID-19 deaths, various ethnic, deprivation score and vaccination rate disparities noted that can adversely affect hospitalization and deaths among compared groups.
CONCLUSIONS There is no discernable vaccine effectiveness among ≥18 years of age, vaccinated third dose population since the beginning of the Omicron variant surge. Pre-existing conditions, ethnicity, deprivation score, and vaccination rate disparities data need to be adjusted for evaluating VE for hospitalizations and deaths. The increased cases with significantly increased hospitalizations and deaths among the elderly population during the Omicron variant surge underscores the need to prevent infections in the elderly irrespective of vaccination status with uniform screening protocols and protective measures.
INTRODUCTION
Following the World Health Organization (WHO), the UK Health Security Agency (UKHSA) designated the Omicron variant (B.1.1.529) of the SARS-CoV2, the virus that causes COVID-19, as a variant of concern on November 27, 20211–3. The Omicron variant spread rapidly across the United Kingdom (UK) and became a predominant strain with 365,375 confirmed cases as of December 23, 20214, 5. UK reported a total of 11.3 million SARS CoV2 cases during the Omicron variant surge in twenty-one weeks as of May 1, 2022 with a majority of the newly confirmed infections of Omicron variant lineages (B.1.1.529 and B.1.1.529.BA.2)6, 7.
The UK COVID-19 vaccination program started in December 2020, with two doses of either mRNA-based vaccines (BNT162b2 and mRNA-1273) or adenoviral vector-based vaccine (ChAdOx1 nCoV-19). Approximately 73.9% of the ≥50 years old population were vaccinated by May 2, 2021 during the beginning of the Delta variant (B.1.617.2) surge8.
After the initial approval the third dose (booster) to only immunocompromised population, the UK authorities approved the third dose to ≥50 years old general population on September 14, 2021 to be administered no sooner than within six months after the primary course9, 10. The third dose vaccination was subsequently expanded in UK to over 18 years old population on November 29, 2021 and changed the booster timing to no sooner than three months after the primary course due to changing risk posed by Omicron variant11. The UK government later announced the fourth dose (booster) in March 2022 12, 13.
While the vaccine immunity was reported waning during the Delta variant surge elsewhere, the initial Public Health England reported a good vaccine effectiveness with two doses of BNT162b2 and ChAdOx1 nCoV-19 vaccine among those with the delta variant (B.1.617.2)14–17. A later study reported waning of effectiveness for symptomatic infections with Delta variant, but limited waning in effectiveness against COVID-19 related hospitalizations and deaths18. During this time, the UK technical briefings also showed a growing problem of breakthrough infection in confirmed Delta variant cases among the ≥50 years age group with 75.3% of breakthrough cases (63.5% of hospitalizations and 67.0% of deaths) as of September 12, 202119–21. Similarly, the weekly vaccine surveillance reports also show a trend of increased cases in the vaccinated third booster population than the unvaccinated population during the Omicron variant surge22. These reports highlight an alarming trend of increased hospitalizations and deaths among the vaccinated third dose population until they stopped reporting the underlying data after March 27, 202222. The UK COVID-19 dashboard is also reporting a relatively higher number of daily hospitalizations and deaths during the later period of the Omicron variant surge in March-April 2022, despite substantially lower cases reported6.
In this Observational study, the changing pattern of SARS-CoV2 cases, hospitalizations and deaths among various age groups during the Omicron variant surge relative to earlier surges was analyzed. We also analyzed SARS-CoV2 cases, hospitalizations and deaths among ≥18 years old population based on the vaccination status during the Omicron variant surge.
METHODS
STUDY DESIGN
In this observational study, we analyzed the nationwide available data of the confirmed SARS-CoV2 cases, hospitalizations and deaths in the UK from the beginning of the COVID-19 pandemic until May 1, 2022. The available data from various UK databases were utilized to study the pattern of cases, hospitalizations and deaths among various age groups during the pandemic. The vaccine effectiveness (VE) was calculated based on the data from UK vaccine surveillance reports, and UK technical briefings until March 27, 2022. We also analyzed the data on racial ethnicity, pre-existing conditions, Indices of Multiple Deprivation (IMD) score and adaptation of SARS-CoV2 vaccination among racial ethnic groups.
DATA SOURCES AND ANALYSIS
Total UK SARS-COV2 cases, hospitalizations and deaths
The following explains our data collection to analyze the number of SARS-CoV2 cases, hospitalizations, and deaths in the UK.
Cases
We analyzed SARS-CoV2 cases reported under pillar 1 (public health laboratories and hospitals) and pillar 2 (community testing) among age groups from September 28, 2020 to May 1, 2022 using the data from National Flue and COVID-19 surveillance reports (2020-2021 season and 2021-2022 season)8, 23.
Hospitalizations
We examined the daily hospitalizations among various age groups from October 12, 2020 to May 1, 2022 using the National Health Services (NHS) database of COVID-19 hospital activity24.
Deaths
We analyzed the weekly SAVRS-CoV2 deaths among various age groups in England and Wales from the beginning of the pandemic in March 2020 to May 1, 2022 using the UK Office for National Statistics dataset25. We compared the weekly SARS-CoV2 deaths among various age groups during each surge with prior surges.
We tabulated and analyzed the changing pattern of cases, hospitalizations and deaths during various surges.
Analysis of the factors known to impact the SARS-CoV2 outcomes
Pre-existing conditions among COVID-19 deaths and COVID-19 deaths among ethnic groups in England: The National Health Services weekly data of COVID-19 deaths archives was used to analyze the pre-existing conditions among COVID-19 deaths in various age groups26.
SARS-CoV2 cases, hospitalizations and deaths among ethnic groups and deprived populations based on IMD score: SARS-CoV2 cases (pillar 1 and pillar 2) per 100, 000 population among various ethnic groups (from June 29, 2020 to May 1, 2022), SARS-COV-2 hospitalizations (excluding ICU/HDU), SARS-CoV2 admission to ICU/HDU units (March 16, 2020 to May 1, 2022), SARS-CoV2 pillar 1 and 2 cases and SARS-CoV2 deaths per 100, 000 population among population-based on Indices of Multiple Deprivation (from June 27, 2020 to April May 1, 2022) were tabulated with weekly data from the National Flu and COVID-19 surveillance reports8. The IMD quintile 1 and decile 1 are considered the most deprived and quintile 5 and decile 10 are the least deprived.
Vaccine uptake among racial minorities
The weekly vaccine uptake data among various ethnic groups was analyzed for the period ending May 1, 20228.
Vaccination data
The National Immunization Management System (NIMS) vaccination data since the beginning of the vaccination program in December 2020 which was published weekly in the National Flu and COVID-19 surveillance reports was used to calculate the vaccinated and unvaccinated population among age groups for a specified period of vaccine effectiveness8. The cases, hospitalizations (cases presenting to emergency care within 28 days of a positive test resulting in overnight inpatient admission) and deaths (within 28 days of a positive COVID-19 test) among various age groups (published weekly) with an aggregate of 4 weeks data since August 14, 2021 to March 27, 2022 periods (for the third dose since December 20, 2021) in the COVID-19 vaccine surveillance reports was used in our analysis of the data22. The Public Health England technical briefings data of cases, hospitalizations and deaths among the confirmed cases of Delta variant was used for data analysis during the period ending June 21, 2021 to August 29, 2021 (included in supplemental appendix)27. The UK Health Security Agencies COVID-19 vaccine surveillance reports did not publish the third dose cases, hospitalizations and deaths until December 19, 2021. We used ≥18 years, pillar 2 cases published by the UKHSA in between November 27, 2021 to January 12, 2022 periods to calculate the vaccine effectiveness of the third dose28. We used over 18 years age groups for vaccine effectiveness as the younger age population was excluded in the randomized controlled trials initially and over 18 years of age was chosen in a recent UKHSA publication28–31. We also analyzed the vaccine effectiveness among over 50 years population for infections. The SARS-CoV2 events (cases, hospitalizations and deaths) tested positive with the specimen date ≥14 days post second dose are considered vaccinated with two doses; the events ≥14 days after receiving third dose are considered vaccinated with the third dose, and the events post one dose without additional doses of vaccination are considered one dose22.
STATISTICAL ANALYSIS
We conducted the statistical analysis using the R software, version 4.1.3. We used the linear regression analysis to test if the total weekly SARS-CoV2 cases (independent variable) in the UK during each surge significantly predicted either hospitalizations or deaths (dependent variables).
We compared the cases, hospitalizations, and deaths among the various age groups between the surges to determine the changing pattern of cases, infections, and deaths during the course of the pandemic. We computed the relative risk (RR), the 95% confidence interval, and the p-value (<0.05 denotes a significant difference between the comparison periods for each age group).
We used the weekly published National Immunization Management System (NIMS) vaccination data to calculate the population for each age group for vaccine effectiveness8. We obtained the number of cases, hospitalizations, and deaths from the vaccine surveillance reports, and the data of these outcomes linked to the NIMS database22. The incidence rate was calculated as a number of SARS-CoV2 infections, hospitalizations or deaths per 100,000 population for each studied group. The incidence rate ratio (IRR) was calculated among the compared groups. The partially vaccinated (received 1 dose), vaccinated with two doses and the third booster were compared with the unvaccinated for the VE calculations. Vaccine effectiveness was calculated as (1-IRR) x 100. We performed the proportions test to determine whether the proportion of cases, hospitalizations, and deaths among the vaccinated population are significantly higher than the unvaccinated population.
RESULTS
United Kingdom SARS-CoV2 cases, SARS-CoV2 hospitalizations and SARS-CoV2 deaths (Figure 1)
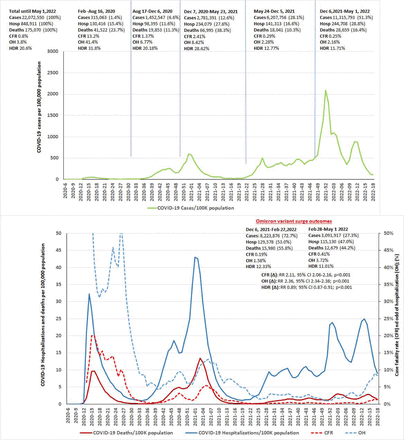
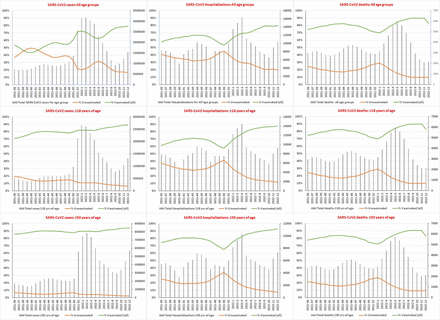
There was a total of SARS-CoV2 cases (n=22,072,550); hospitalizations (n=848,911) and deaths (n=175,070) reported in the UK during the entire pandemic as of May 1, 2022. The majority of cases (51.3%; n=11,315,793), majority of hospitalizations (28.8%; n=244,708) and second-highest percentage of deaths (16.4%; n=28,659) occurred in twenty-one weeks period during the Omicron variant surge in our study (December 6, 2021 to May 1, 2022).
Total SARS-CoV2 cases, hospitalizations, and deaths in UK during the entire COVID-19 pandemic until May 1, 2022. The graph illustrates the increasing odds of the hospitalization (OH) and case fatality rate (CFR) during the latter part of the Omicron variant surge. The OH and CFR significantly increased during the latter part of the Omicron variant surge (February 27-May 1, 2022) mainly driven by increased hospitalizations and deaths despite the lower number of cases.
The case fatality rate (CFR) of 13.2% and the odds of hospitalization (OH) of 41.4% were highest during the first wave (February 24-August 16, 2020); during the Alpha variant surge the CFR was 2.41% with OH of 8.42%. The CFR and OH decreased to 0.29% and 2.28%, respectively during the Delta variant surge and the lowest CFR of 0.25% and OH of 2.16% was observed during the Omicron variant surge. The CFR (0.19% vs 0.41%; RR 2.11, 95% CI 2.06-2.16, p<0.001) and OH (1.58% vs 3.72%; RR 2.36, 95% CI 2.34-2.38; p<0.001) significantly increased during the 9 weeks period ending May 1, 2022 in the latter part of the Omicron variant surge compared to the earlier 12 weeks.
The regression analyses of SARS COV-2 cases, hospitalizations, and deaths (all age groups outcomes for UK) demonstrated a strong correlation between the number of cases (independent variable), and the numbers of hospitalizations and deaths as shown on Figure S1 (details of analysis included in the supplementary appendix).
SARS-CoV2 cases, SARS-CoV2 Hospitalizations (in England) and SARS-CoV2 deaths (England and Wales) among age groups (Figures 2a-c; Tables S1a-c)
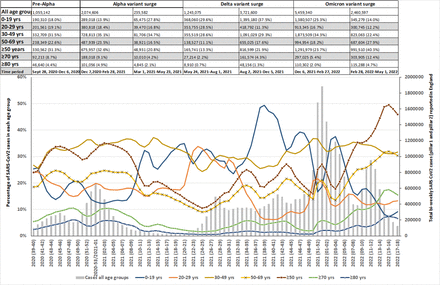
Analysis of the SARS-CoV2 cases in England among various age groups showed a significantly increased percentage of cases among ≥50 years age group during the initial part of the Omicron variant surge (21.9% vs 23.7%; RR 10.07; 95% CI 1.07-1.08);p<0.001) and during the latter part of Omicron variant surge (23.7% vs 40.3%; RR 1.70;95% CI 1.70-1.71;p<0.001) compared to immediate prior period as shown on the Table S1a particularly among ≥70 years age of age. During the same periods in England, there were significantly increased hospitalizations among ≥75 years age group during the initial (30.8% vs 39.2%; RR 1.27;95% CI 1.25-1.29;p<0.001) and the latter part of Omicron variant surge (39.2% vs 50.3%;RR 1.28;95% CI 1.27-1.30;p<0.001). The SARS-CoV2 deaths in England and Wales during this time revealed significantly increased deaths during the initial part of the Omicron variant surge among 70-74 years (11.58% vs 16.02%; RR1.38;95%CI 1.30-1.47;p<0.001) and ≥75 years age group (59.33% vs 67.89%; RR1.14;95%CI 1.12-1.17;p<0.001). During the latter part of Omicron variant surge ≥75 years age group have significantly increased deaths (67.89% vs 80.07%; RR1.18;95%CI 1.16-1.20;p<0.001) and 70-74 years age group showed significantly decreased deaths (16.02% vs 7.69%; RR 0.48;95% CI 0.44-0.52);p<0.001). The hospitalization and deaths significantly decreased in <75 years of age with associates decreased cases in <50 years of age during the latter part of Omicron variant surge.
SARS-CoV2 cases (pillars 1 and 2) in England among various age groups in England from September 28, 2020 to May 1, 2022. The number of cases during the various surges is shown on the top panel for each age group (n=; %) and the percentage of two weekly cases among each age group is shown on the graph. As shown, there was an increased percentage of cases noted among ≥50 years of age groups (that was noted to be statistically significant as shown in Table S1a) during the latter part of the Omicron variant surge during the February 28-May 1, 2022 period. The percentage of cases among <50 years of age groups significantly decreased during the same period as shown in Table S1a.
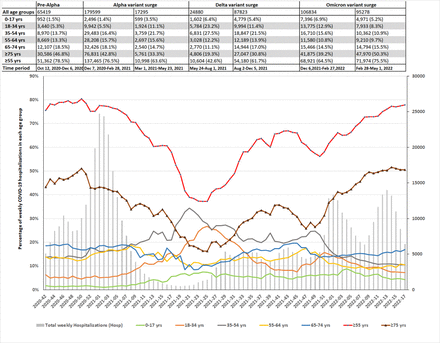
SARS-CoV2 hospitalization in England among various age groups in England from October 12, 2020 to May 1, 2022. The number of hospitalizations during the various surges is shown on the top panel for each age group (n=; %) and the percentage of weekly hospitalizations among each age group is shown on the graph. As shown, there was an increased percentage of hospitalizations noted among ≥75 years of age groups (that was noted to be statistically significant as shown in Table S1b) during the latter part of the Omicron variant surge during the February 28-May 1, 2022 period. The percentage of hospitalizations among <55 years of age groups significantly decreased during the same period as shown in Table S1b.
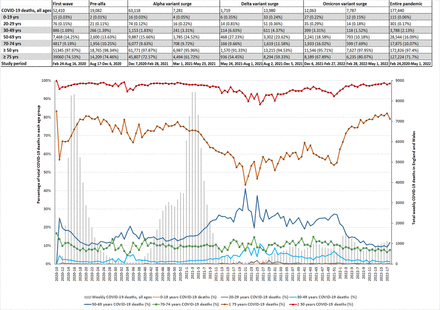
SARS-CoV2 deaths in England and Wales among various age groups from February 24, 2020 to May 1, 2022. The number of deaths during the various surges is shown on the top panel for each age group (n=; %) and the percentage of weekly deaths among each age group is shown on the graph. As shown, there was an increased percentage of deaths noted among ≥75 years of age groups (that was noted to be statistically significant as shown in Table S1c) during the latter part of the Omicron variant surge during the February 28-May 1, 2022 period. The percentage of deaths among <75 years of age groups significantly decreased during the same period as shown in Table S1c.
SARS-CoV2 cases, hospitalizations, ICU admissions and deaths among ethnic groups and deprived populations based on IMD score in England (Figures 3a-e)
SARS-CoV2 cases and hospitalizations per 100,000 were highest in ethnic minorities than in the white ethnic group during and prior to the Alpha variant surge, the initial part of the Delta and Omicron variant surges. The case rates and hospitalization rates among the white ethnic group increased during the latter part of the Delta variant surge and the latter part of the Omicron variant surge from February 28-May 1, 2022. However, the white ethnic group have lower ICU/HDU admission rates during the entire pandemic since March 2020. The cases per 100,000 population among the most deprived (IMD score) have higher case rates than the least deprived during the Alpha and initial part of Delta and Omicron variant surges, while the least deprived have higher rates of cases during the latter part of Delta and particularly during the latter part of Omicron variant surge (February 28-May 1, 2022). However, the death rate among the most deprived is higher than the least deprived all throughout the pandemic, although the gap is narrowing during the latter part of the Omicron variant surge.
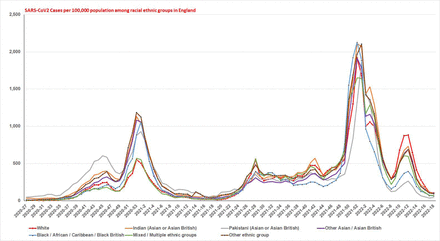
Weekly SARS-CoV2 cases (pillars 1 and 2) per 100,000 population among various ethnic groups in England from June 29, 2020 to May 1, 2022. As shown in the graph, racial minorities have higher infection rates period to and during the alpha variant surge, during the initial part of the Delta and Omicron variant surges than the white ethnic group. During the latter part of the Delta and Omicron variant surges, the white ethnic group have higher infection rates than other minorities.
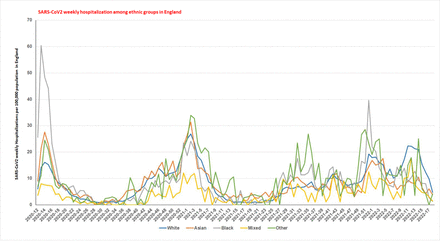
Weekly SARS-CoV2 hospitalizations per 100,000 population among various ethnic groups in England from March 16, 2020 to May 1, 2022. As shown the graph, racial minorities (black, Asian, mixed and other) have higher hospitalization rates during the First wave, the Alpha variant surge, and during the Delta variant surge. During the initial part of the Omicron variant surges racial minorities (black and other) have higher rates of hospitalization than the white ethnic group. During the latter part of the Omicron variant surges, the white ethnic group hospitalization rates increased.
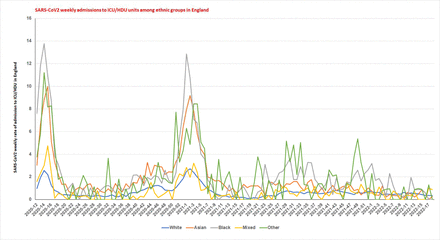
Weekly SARS-CoV2 admissions to ICU/HDU per 100,000 population among various ethnic groups in England during the March 16, 2020 to May 1, 2022. As shown, the racial minorities have higher rates of admission to ICU/HDU during the entire COVID-19 pandemic compared to the white ethnic group.
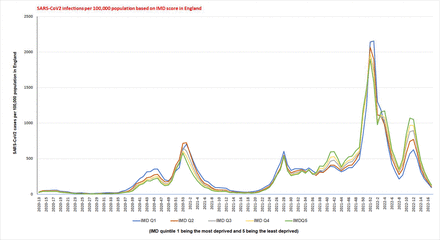
Weekly SARS-CoV2 cases (pillars 1 and 2) per 100,000 population based on the Indices of Multiple Deprivation (IMD) from March 16, 2020 to May 1, 2022. The infection rates were higher in most derived during the entire pandemic, except during the latter part of the Delta variant and particularly the latter part of the Omicron variant surge. During the latter part of the Omicron variant surge, the infection rates of the least deprived are higher than most deprived.
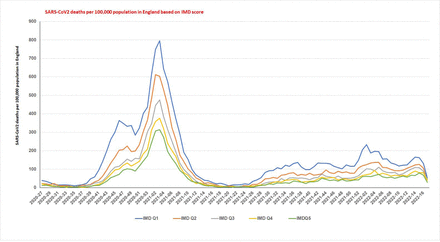
Weekly SARS-CoV2 deaths per 100,000 population based on the Indices of Multiple Deprivation (IMD) from March 16, 2020 to May 1, 2022. The death rates were higher in most derived during the entire pandemic including the latter part of the Omicron variant surge than the least deprived.
SARS-CoV2 deaths among age groups in England and pre-existing conditions (Table S2)
The pre-existing conditions are present in 95.6% of COVID-19 deaths among all age groups (96.2% among those ≥60 years of age, 90.6% among 40-59 years, 82.8% among 20-39 years and 69.2% of deaths among 0-19 years of age) during the Omicron variant surge.
Vaccination rates among ethnic groups and population based on deprivation score (IMD) as of May 1, 2022 (Table S3b)
The NIMS database of over 18 years, the British white have the highest third dose vaccination rate of 76.4%, lower rates of receiving two doses without a third dose (12.5%) and lowest rates of unvaccinated rate (8.9%). The population considered least deprived based on IMD decile score have the highest third dose vaccination rate (86.7%), lower rates of two doses only without third dose (10.2%) and lowest unvaccinated rate (1.4%); while the most deprived have lowest third dose vaccination rate (55.2%); higher rates of two doses without third dose (25.2%) and unvaccinated rate (13.9%). The racial minorities have lower percentage of third dose vaccination (33-55%), higher rates of not receiving third dose after 2 doses (21.2%) and highest rate of unvaccinated (28.8%).
Outcomes among ≥18 years of age NIMS vaccinated population in UK (Figures 4–6, Table S3a, Tables S5a-c; Tables S6a-c, Tables S7a-c, Tables S8a-f)
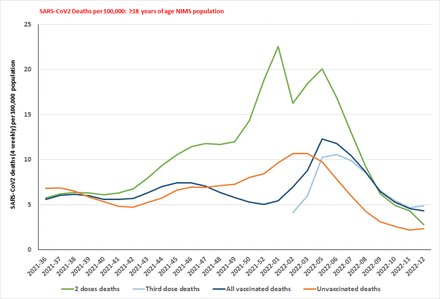
The data published in UK vaccine surveillance reports (August 16, 2021-March 27, 2022) was used for the analysis. The ≥18 years of age two doses vaccinated population showed vaccine effectiveness of 17.5% (95% CI 16.5%-18.4%) for the four weeks period ending September 12, 2022. Ever since, the vaccinated with two doses and the third dose (since December 20, 2021) have negative vaccine effectiveness with the vaccinated population having a greater proportion of cases than the unvaccinated. The UKHSA did not report third dose outcomes until December 20, 2021 in their weekly reports. In our study, we analyzed the 336,046 cases among the third booster pillar 2 population (November 27, 2021-January 12, 2022) and using the third dose weekly vaccinated population between December 26, 2021 to January 9, 2022, the best vaccine effectiveness for the third dose was 13.8%, 18.4%, and 22.2%, respectively. The proportion test showed that the all-vaccinated population have higher proportion of cases than the unvaccinated since August 23, 2021 (X2 = 11.686, df = 1, p = 0.0003149) and since the third dose reporting period of December 20, 2021 (X2= 79651, df = 1, p<0.001). Of the vaccinated populations, the vaccinated with two doses have significantly higher proportion of cases since August 30, 2021. Since January 31, 2022; the third dose vaccinated population have significantly higher proportion of cases than two doses (X2= 368.53, df = 1, p<0.001) and unvaccinated (X2= 55147, df = 1, p<0.001). The proportions test also showed that over 18 years old two doses vaccinated population have significantly higher proportion of hospitalizations than unvaccinated (X2= 332.3, df = 1, p<0.001) since December 6, 2021 and since January 17, 2022 all vaccinated population have significantly higher proportion of hospitalizations than unvaccinated (X2= 14.103, df = 1, p<0.001). Since January 24, 2022, the third dose population also have a higher proportion of hospitalizations than unvaccinated (X2= 33.446, df = 1, p<0.001). Since February 14, 2022 the third dose population have higher proportion of hospitalizations than two doses (X2= 25.946, df = 1, p<0.001) and unvaccinated (X2= 121.11, df = 1, p<0.001). The proportion test on deaths also showed a significantly higher proportion of deaths among vaccinated over 18 years old with two doses than unvaccinated since September 13, 2021 (X2= 7.6872, df = 1, p = 0.0028), all vaccinated population higher proportion of deaths than unvaccinated since January 10, 2022 (X2= 41.017, df = 1, p<0.001) and third dose higher (X2= 53.465, df = 1, p<0.001) than unvaccinated since January 17, 2022. Since, February 14, 2022, the vaccinated population with third dose had a higher proportion of deaths versus the vaccinated with two doses (X2= 2.8687, df = 1, p p<0.001) and unvaccinated (X2= 122.59, df = 1, p<0.001). The significantly increased proportion of cases in the vaccinated population during the Omicron variant was associated with significantly increased hospitalization and deaths among vaccinated population of ≥18 years of age with significant decreased cases, hospitalizations and deaths in unvaccinated.
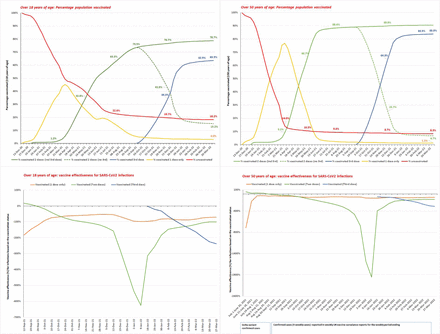
The vaccination rates of over 18 years of age (top left), and over 50 years of age (top right); the vaccine effectiveness of over 18 years of age (bottom left) and over 50 years of age (bottom right) during the Delta variant sure and the Omicron variant surge until March 27, 2022. The top panel shows the percentage of the population vaccinated during the vaccination program weekly (for the week ending) until March 27, 2022. The bottom panel shows vaccine effectiveness for rolling four weekly cases from August 16, 2021 until March 27, 2022 (rolling 4 weeks ending date on x-axis). The ≥50 years of age Delta variant cases vaccine effectiveness (bottom right graph), the dates are listed on x-axis. Table S3a shows detailed vaccination rates of NIMS population (all ages, over 18 years and over 50 years of age groups) and Table S3b shows the vaccination rate disparities of the ethnic groups and vaccination disparities based on the IMD score. Table S7a-c shows the vaccine effectiveness (95% CI), of ≥18 years and ≥50 years of age NIMS population including the Delta variant cases vaccine effectiveness of ≥50 years of age.
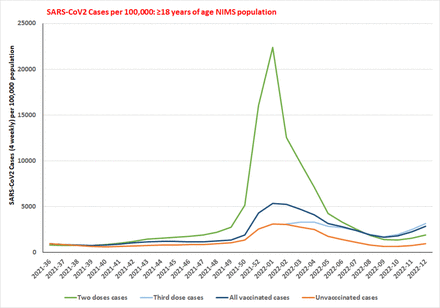
SARS-CoV2 cases per 100,000 population among over 18 years of age group from August 16, 2021 to March 27, 2022. Table S8a shows that the vaccinated population (including two doses) have a significantly higher proportion of cases than the unvaccinated during the latter part of the Delta variant and initial part of Omicron variant surges. During the latter part of the Omicron variant surge, the vaccinated with the third dose have the highest proportion of infection than those vaccinated with two doses and unvaccinated.
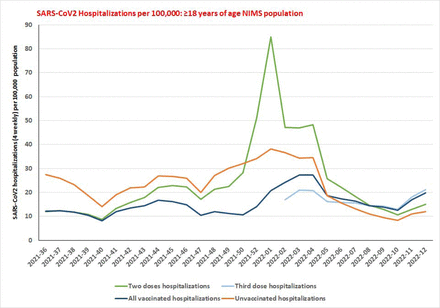
SARS-CoV2 hospitalizations per 100,000 population among over 18 years of age group from August 16, 2021 to March 27, 2022. Table S8b shows that the vaccinated with two doses have a significantly higher proportion of hospitalizations than the unvaccinated during the initial part of the Omicron variant surge. During the latter part of the Omicron variant surge, the vaccinated with the third dose (including all vaccinated population) have the highest proportion of hospitalizations than those vaccinated with two doses and unvaccinated.
SARS-CoV2 deaths per 100,000 population among over 18 years of age group from August 16, 2021 to March 27, 2022. Table S8c shows that the vaccinated population with two doses has a significantly higher proportion of hospitalizations than the unvaccinated during the latter part of the Delta variant surge and the initial part of the Omicron variant surge. During the latter part of the Omicron variant surge, the vaccinated with the third dose (including all vaccinated population) have the highest proportion of deaths than those vaccinated with two doses and unvaccinated.
The percentage of SARS-CoV2 cases (left), hospitalizations (middle) and deaths (right) based on the vaccination status among all age groups (top row) over 18 years of age (middle row) and over 50 years of age (bottom row) reported from the NIMS database from August 16, 2021 to March 27, 2022. The detailed rolling four weekly changes the percentage of SARS-CoV2 cases (Table S6a), SARS-CoV2 hospitalizations (Table S6b) and SARS-CoV2 deaths (Table S6c) are shown the tables. The increased SARS-CoV2 cases among the vaccinated population in each age group during the Omicron variant surge is associated with increased SARS-CoV2 hospitalizations and SARS-CoV2 deaths in the vaccinated population. The decreased SARS-CoV2 cases among the unvaccinated population in each age group during the Omicron variant surge is associated with decreased SARS-CoV2 hospitalizations and SARS-CoV2 deaths in unvaccinated. The proportionality test results detailed in Tables S8(a-f); show that a significantly higher proportion of SARS-CoV2 cases in the vaccinated population (including the third dose) than in unvaccinated during the Omicron variant surge was associated with a significantly higher proportion of SARS-CoV2 hospitalizations in all vaccinated population (including the third dose) than the unvaccinated among ≥18 years of age and ≥50 years of age during the latter part of the Omicron variant surge. The proportionality test also shows a significantly higher proportion of deaths among ≥18 years of age vaccinated population (including the third dose) than unvaccinated during the latter part of Omicron variant surge. The proportionality test also showed higher proportion of deaths among ≥50 years of age vaccinated with two doses than unvaccinated during the Omicron variant surge with the third dose population deaths lower than unvaccinated until March 27, 2022.
The detailed analysis of ≥50 years of age vaccinated population and analysis of changing pattern of cases, hospitalizations and deaths among various age groups tabulated in the supplemental appendix.
DISCUSSION
There was a total of 22.07 million SARS-CoV2 cases; 848,911 hospitalizations and 175,070 deaths reported in UK during the pandemic as of May 1, 2022. The highest percentage (51.3%) of the cases, highest percentage (28.8%) of hospitalizations, second highest percentage of deaths (16.4%) occurred during the Omicron variant surge in 21 weeks until May 1, 2022. The Alpha variant surge reported highest percentage (38.3%) of deaths in 25 weeks, with 10.3% of total deaths and the second highest percentage of cases (28.1%) occurred during the Delta variant surge in 27 weeks. Omicron variant surge was associated with lower case fatality rate and lower odds of hospitalizations than the Delta variant during the first twelve week until February 27, 2022 in our study; a similar finding was reported in a recent study for the period ending January 9, 202232. We observed increased case fatality rates and odds of hospitalizations during the latter part of Omicron variant surge, which was higher than what was observed during the Delta variant surge. We also noted increased cases among ≥50 years age groups associated with significantly increased hospitalizations and deaths particularly in ≥75 years age group (80.1% of total deaths) after February 27, 2022. A similar pattern of significantly increased SARS-CoV2 cases and hospitalizations in over 50 years old population was associated with a significantly increased deaths among ≥70 years old age group during the latter part of the Delta variant surge in UK33.
The ≥18 years of age NIMS population in our study showed waning of vaccine effectiveness for the two doses during the Delta variant surge (since September, 2021) with the vaccines effectiveness for the infections is in the negative during the Omicron variant surge in all the vaccinated groups including the third dose population since the December 20, 2021. In this analysis the cases reported in a UKHSA publication that showed a 22.2% best possible effectiveness for the third dose during the November 27, 2021 to January 12, 2022 period. The proportion test showed significantly higher proportion of infections in vaccinated with two doses (including all vaccinated) than unvaccinated during the Delta variant surge (since September 2021). Additionally, the vaccinated with third dose had significantly higher infection rates than vaccinated with two doses and unvaccinated during the Omicron variant surge (since February 2022). This was associated with a significantly higher proportion of hospitalizations in vaccinated with two doses than unvaccinated during the Omicron variant surge (since January 2022), higher proportion of deaths in vaccinated two doses than unvaccinated (since October 2021) and higher proportion of hospitalizations and deaths in vaccinated with third dose than vaccinated with two doses and unvaccinated during Omicron variant surge (since February 2022).
The NIMS database also clearly shows the disparities of the vaccination rates with British white and least deprived per IMD decile score (vaccinated with highest percentages of the third dose) have the lowest infection rates, hospitalizations and deaths due to COVID-19 even before the vaccination. The ethnic minorities and the most deprived based on IMD decile score (have lowest rates of third booster vaccinations, highest rates receiving only two doses without the booster and highest rates of unvaccinated compared to British white) also had higher infection rates, hospitalizations and deaths due to COVID-19 from the beginning of the pandemic. In our analysis of the data, the pre-existing conditions that were associated with 95.8 to 96.8% of deaths among over 60 years old population in England during the Omicron variant surge until May 1, 2022. The pre-existing conditions were also reported in the majority of COVID-19 deaths during prior surges including Delta variant surge34. The racial disparities with increased deaths due to COVID-19 among ethnic minorities compared to white British population were reported in multiple UK Office for National Statistics publications from beginning of COVID-19 pandemic in 2020 until recent publication on April 7,202235–38. Other studies have also shown that increased infections, hospitalizations and deaths noted among racial minorities in UK39, 40.
Based on the analysis, the vaccination groups (third dose, two doses only and unvaccinated) have heterogenous populations that have different known infection rates, hospitalizations and deaths due to COVID-19 dating back to the beginning of the pandemic way before UK started vaccination program in December 2020. In the light of these known variables, SARS-CoV2 cases among the compared groups for vaccine effectiveness can be adversely affected by the behavior of population and or opportunity for exposure either at home or at work based on the density of population16, 41–43. Additionally, all the scientific evidence shows that in additional to increased cases and age, the vast majority of hospitalizations and deaths were associated with pre-existing conditions especially in elderly population34, 44–46. In our study, increased cases predicted higher hospitalizations and deaths among all reported cases in UK and our study also demonstrated changes in proportion of cases among various age groups during surges were associated with similar changes hospitalizations and deaths particularly in elderly. Based on these known variables, the vaccine effectiveness for the hospitalizations and deaths need to be adjusted for increased cases due to behavior or exposure risk; other known variables (racial ethnicity, deprivation score) and must be adjusted for pre-existing conditions especially in elderly.
The waning vaccine effectiveness in our study is based on the traditional vaccine effectiveness (1-RR), is different than various UK publications. During the Delta variant surge, while the two UK publications using test-negative case-control design reported good outcomes, the Public Health England technical briefings showed increasing cases of confirmed COVID-19 Delta variant cases in the ≥50 years age group, with fully vaccinated (two doses) share of breakthrough cases increased from 37.0% for the period ending June 21, 2021 to 75.3% of breakthrough cases (63.5% of hospitalizations and 67.0% of deaths) as of September 12, 202119–21. The UK vaccine surveillance reports using a similar methodology also project good vaccine effectiveness for the hospitalizations and death during the Omicron variant surge (until May 1, 2022 study period) even when the infection rates of the third dose were higher than the unvaccinated and vaccinated with two doses22. In the absence of vaccine effectiveness to prevent COVID-19 infections, it is scientifically sub-optimal to project good vaccine effectiveness for hospitalizations and deaths without adjusting the data for all known variables (published by UK health agencies in their regular weekly reports) that can independently affect these outcomes. This practice of unadjusted and unvalidated projections of good vaccine effectiveness for the hospitalizations and deaths (when cases are increasing in vaccinated than unvaccinated without vaccine effectiveness) may create a false sense of security and harm the vaccinated population if they do not take adequate precautions to avoid infection. This is more relevant in the view of studies showing decreased vaccine effectiveness among the elderly population which is the same age group that is at the highest risk for increased hospitalizations and deaths18, 47.
The decreased cases among the unvaccinated population during the Omicron variant surge is probably due to protection from their prior natural infections that was already shown to give lasting immunity which need further study48, 49. The deferent vaccine effectiveness methodologies used by the Israeli (traditional vaccine effectiveness) and UK (test-negative case-control design) health officials are probably the main reasons for discordance between Israeli data that led to the early approvals of third dose on July 30, 2021 (Delta variant surge) and fourth dose on December 21, 2021 (Omicron variant surge) while the UK data is still showing favorable vaccine effectiveness using test-negative case-control design especially for hospitalizations and deaths which needed to be further studied14, 17, 18, 50, 51.
The strength of our investigation is the comprehensive analysis of nationwide real-world data of the various variables associated with SARS-CoV2 infections, hospitalizations and deaths in the UK during the entire pandemic. Our analysis also identified heterogenicity vaccinated (two doses or third dose) and unvaccinated populations that had variabilities in infection rates, hospitalizations, and death rates from the beginning of the pandemic which needed to be adjusted for vaccine effectiveness. The findings in this study are similar to recent study in Israel showing increasing breakthrough infections with waning of vaccine effectiveness in elderly population who are considered immune (mostly third dose booster population) were associated with increased severe illness and deaths during the Omicron variant surge42.
One limitation of our study is that it is an observational study of publicly reported data and the generalizability of the findings is limited to the population studied in UK. However, our findings have validity as reflected by UKHSA publication only reporting protection against mild disease during the initial stages of the Omicron variant surge and the actions of the UK authorities to recommend the fourth dose later during the Omicron surge 12, 13.
CONCLUSIONS
There was no discernable vaccine effectiveness to prevent infections among the third dose ≥18 years of age population since December 20, 2021 during the initial part of the Omicron variant surge in UK. The increased SARS CoV2 cases in the vaccinated population (including the third dose) among over 18 years of age during the Omicron variant surge were associated with significantly hospitalizations and deaths, while decreasing cases in unvaccinated population associated with decreased hospitalizations and deaths. Our data analysis identified heterogenous vaccinated (third dose, received two doses without booster) and unvaccinated populations with well-known variables that can increase risk for the hospitalizations and deaths based on ethnicity, deprivation score and pre-existing conditions; and the vaccine effectiveness for hospitalizations and deaths should be adjusted for these variables. Despite decreased total cases in UK, there were significantly increased case fatality rate and odds of hospitalization during the latter part of the Omicron variant surge (February 28-May 1, 2022) in our study which was due to significantly increased cases among ≥50 years of age associated with significantly increased hospitalizations and deaths among ≥75 years of age. This underscores the importance of the public health measures directed at uniform screening protocols, and protective measures to prevent infection among elderly vaccinated and unvaccinated populations.